Covid-19 Information
The safety, health, and wellbeing of our patients, staff, and specialists are of utmost importance to us. Currently, everyone coming to Mercy Hospital is required to practice good hand hygiene.
If you have had Covid-19 since receiving your surgery date, please contact your surgeon to check that this date is still appropriate. For some procedures, evidence suggests it is best to defer surgery following recovery from Covid-19.
For further information, please refer to Covid-19 Information for Patients.
Planning for Surgery
Planning for Surgery
Once you have seen your surgeon and it has been decided that you are to have surgery at Mercy, staff at your surgeon's rooms will give you either a physical or electronic admission pack. This pack includes important information for you to read and a hospital admission form that you need to complete and send back to us before your surgery date.
Electronic admission forms can be submitted using your mobile phone or computer. If returning paper admission forms please allow enough time for postage.
If you require an interpreter this can be arranged by the Credentialed Specialist prior to your admission. Members of your whanau/family who may accompany you through your procedure are not generally the preferred option as an interpreter.
Lab Testing Before Admission
Lab Testing Before Admission
- travelled to selected countries^ - see list below
- OR have stayed overnight in a health care facility overseas or the North Island of New Zealand
- OR live at Birchleigh Residential Care Centre,
you must be tested for Multi-Drug Resistant Organisms (MDROs). MDRO stands for multidrug-resistant organism. MDRO germs can cause infections but they can't be killed by many of the antibiotics that doctors use to treat infections. This makes infections with MDROs harder to treat.
- India
- Pakistan
- Sri Lanka
- Bangladesh
- Nepal
- Bhutan
- Afghanistan
- Vietnam
- Thailand
- Cambodia
- Myanmar
- Laos
- Indonesia
If you have been given a laboratory form in case you require a blood transfusion, this blood test needs to be done no more than 72 hours prior to your surgery.
Pre-admission Process
Pre-admission Process
Almost all patients who come into Mercy Hospital for an operation can expect to receive a telephone call from one of our preadmission nurses. The phone call will last for around five to 15 minutes. Discussion will include requesting information about your current health status, medications and any drug or food allergies.
The nurse will also discuss and follow up on support you have put in place for once you have been discharged home. This is a good time to start thinking of your discharge plan. Please refer to our planning for discharge information to assist you in your planning.
Most patients who are being admitted to Mercy will also be contacted by their anaesthetist and in some situations by their surgeon prior to surgery. This may be in person or by phone. Additionally, if required you may receive a pre-admission phone call from your occupational therapist to discuss your discharge requirements or a phone call from your physiotherapist to discuss rehabilitation and exercise requirements.
If you are attending a pre-admission appointment in person, please visit Mercy Hospital Reception on arrival and staff will direct you to the appropriate area. In person pre-admission appointments may take an hour to an hour and a half.
Following the pre-admission phone calls or appointment with your anaesthetist, you should know:
- The time you need to arrive at the Hospital for your surgery.
- When you need to stop eating and drinking.
- What medications you should be taking on the day of your surgery.
- Requirements for showering.
Please note that Mercy Hospital does not organise convalescent care, however we may be able to put you in touch with support services who can help.
If you need assistance getting to and from Mercy Hospital, the St John’s Health Shuttle may be able to help. Days of operation can be found at https://www.stjohn.org.nz/what-we-do/community-programmes/health-shuttles-stjohn/, or you can call 0800 103 046 for the South Island service.
We have also prepared a pre-admission checklist (below) to assist you in preparing for your stay, as well as a planning for discharge checklist.
Pre-admission Checklist
-
Make sure you have read the following sections of our website, and ask a friend or family member who will be supporting you to read it too:
'Getting prepared for surgery - what to organise in advance.'
'Planning for discharge.' - Paperwork
-
Complete the Patient Admission Form (either electronically or paper copy).
-
Complete the Pharmacy Information Form. (If you hold a Community Services Card, Pharmaceutical Subsidy Card or SuperGold Card please advise on this form.)
-
Obtain a list of all current medications from your pharmacist and bring the list and the medications with you to Hospital.
- Please return this completed paperwork to Mercy Hospital. It is important that we receive these forms at least one week prior to your surgery date. Please allow two weeks for postage.
-
Check any specific pre-admission instructions from your specialist.
-
Plan for support following your discharge. For example, you will need someone to stay with you for the first 24 hours (or longer depending on surgery type), you can pre-prepare meals, arrange for someone to help to feed / walk pets.
-
Arrange transport to and from the hospital (discharge time is 10.00 am - 11.00 am).
-
Pack everything you need to bring including all the medications you are currently taking. Please ask your pharmacist to dispense the medications in their original containers/boxes - blister packs cannot be accepted. (Refer to the 'what you need to pack' section below.)
- When completing your admission forms, you will be given the choice of staying in a single or shared room. We will make every effort to accommodate your preference, but this will depend on availability.
Staying Safe From Infection
Staying Safe From Infection
Most surgical wounds heal without any problems. In a few people, they can develop an infection. This is called a surgical site infection. Your surgeon and everyone working in the hospital will do specific things to ensure your risk of infection is as low as possible.
There are some things you can do before and after surgery to help. Below is a short video that explains what you and your family and whānau can do to prevent an infection developing in your wound when you have surgery.
Te reo Māori and Samoan versions of the video are here:
What You Need to Pack
What You Need to Pack
-
Copy of your current medications from your Pharmacist.
-
All medicines and inhalers (in original containers/boxes - not blister packs) that you are currently using or have recently taken.
Stay over patients at Mercy Hospital
If you are staying overnight or longer, bring along with you the following (in addition to the above):
-
Slippers with non-slip soles.
-
Loose fitting comfortable daywear and nightwear - a change or two depending on how many days you will be staying. Wearing your own clothes during the day in hospital helps prepare you for managing dressing at home.
-
Toiletry requirements and other personal necessities.
-
Items that you usually use or may have been given to use by an Occupational Therapist such as “helping hand” or sock applicator and your patient activity sheet if your surgeon has provided you with one of these.
Patients: Please do not leave your vehicle in the car park or bring valuables with you to the Hospital.
Mercy Hospital is unable to take responsibility for the security of these items.
Children at Mercy
Children at Mercy
Children are admitted to Mercy Hospital through the Coolock Day Surgery Unit (DSU). You will meet the nurse who will be caring for your child. A parent / guardian can accompany your child into theatre and stay with them until they are asleep. Following surgery and recovery, your child will return to the day surgery unit if they are a day case, or to the McAuley Ward if they are staying the night. If your child is staying overnight they may have a tube in their arm that will allow nurses to give pain relief as required.
Please bring your child's:
-
Comfortable clothing / pyjamas (if staying overnight).
-
Special toy, blanket or book.
-
Own toiletries (including nappies if needed).
-
Inhalers or regularly used medications.
-
Bottles, formula or drinking cup if required.
Accommodation for parent / guardian
Accommodation in a recliner chair (that can pull out into a bed) is complimentary for one parent when a child aged 16 or under is required to stay overnight.
To comply with fire safety regulations and to ensure patient safety, we are unable to accommodate a parent in a bed unless a double room is available.
For children aged 17 years and over, a fee will be charged for a parent who requests to stay overnight.
To request overnight accommodation for a child aged 17 years or over as a parent/guardian, please contact our bookings team.
Visiting hours
Parents/whanau are welcome to visit their child at any time.
Planning for Discharge
Planning for Discharge
-
You need to arrange to have a responsible adult stay with you for the first 24 hours (or longer depending on surgery type) after your surgery, or arrange to stay with family or friends. If this is not possible, you will need to consider and arrange an alternative.
-
For those who provide care for other dependents, you may need to consider making alternative arrangements in the short term.
-
Preparing meals ahead of your admission and freezing them can make it easier to manage when you return home.
-
If you will need to use crutches or your mobility is going to be affected by your surgery, think about the placement of furniture and rugs at home. The location of everyday items such as saucepans and crockery may need to be changed ahead of your return home.
-
Many people are surprised at the time it takes to recover from an operation even if it is a minor procedure. It is common to feel tired and you may need to set aside some time in the day to rest.
-
Please make sure you have arranged for a relative or friend to drive you home from the hospital on the day you are discharged, you will not be able to drive yourself.
Physiotherapy
Physiotherapy
Physiotherapy is available for pre-operative exercises and mobility advice. This is combined with education for your specific surgery. Telehealth consultations are available.
For a consultation at Mercy's Physiotherapy Clinic: phone 03 464 0107, or contact our physiotherapy clinic via our feedback form here.
Hip and knee joint replacements:
Classes are available before your hip or knee joint replacement surgery. The class covers information regarding your recovery, exercises and any equipment that may be needed after your surgery. The classes are taken by the Mercy Allied Health team and are every second Thursday of the month, 1:00pm - 2:00pm at Marinoto House, Mercy Hospital.
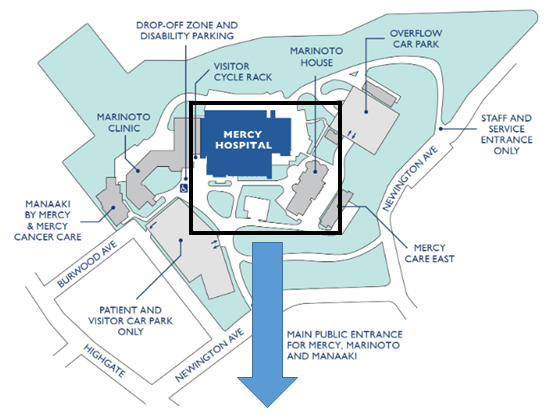
Where to find the class:
Allied Health Pre-Operative Class
Thursday 1 P.M.
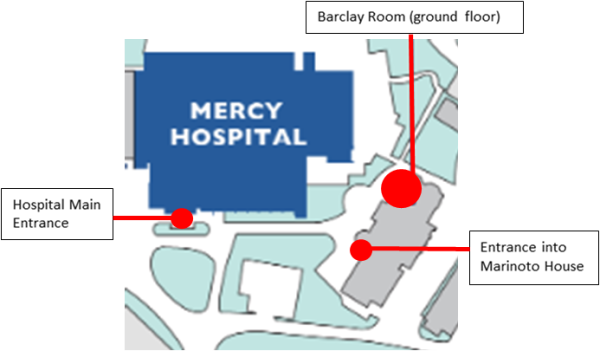
Please go to Barclay Room, ground floor of Marinoto House, See below:
To book your class session before your joint replacement surgery, please phone 03 464 0107 or use the booking tool below:



